Introduction
Mosquitoes are one of the most important insect pests that affect the health and wellbeing of humans and domestic animals worldwide. They can cause a variety of health problems due to their ability to transfer (vector) viruses and other disease-causing pathogens even in the arid Southwest. Female mosquitoes require a blood meal for egg production, and they can produce a painful bite as they feed. While feeding they can transmit to humans and other animals─brain inflammation (encephalitis), dengue fever, yellow fever, malaria and filariasis. The most susceptible to the effects of these mosquito-borne pathogens are children and the elderly. However, in some instances life-threatening illness and/or permanent debilitation can occur in infected human hosts of any age.
The Mosquito Life Cycle
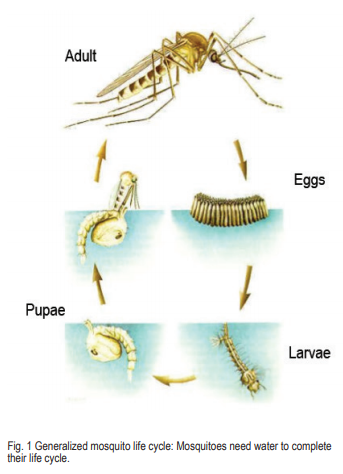
Understanding the basics of mosquito biology will help to reduce mosquito problems. All mosquitoes must have water to complete their life cycle, although some species require very little water and can develop in a thin moisture film. The mosquito life cycle is an example of complete metamorphosis. There are four distinct stages in the life of a mosquito: egg, larva (aquatic feeders), pupa (aquatic nonfeeders) and adult (Fig. 1). Like most insects with complete metamorphosis, mosquitoes have developmental stages that look very different from one another.
They begin life as tiny eggs. Female mosquitoes usually lay eggs a few days after acquiring a blood meal. Depending on the species the eggs can be laid either singly (e.g. Aedes aegypti, Fig. 2A) or in rafts (e.g. Culex mosquitoes) (Fig. 2B). The eggs are laid on the surface of water, on the sides of containers, or on damp soil.
The eggs hatch into squiggly little larvae or “wrigglers” that swim in the water and feed on microorganisms or decaying organic matter. A larva goes through four growth stages called instars, in which they grow in size, before reaching the relatively inactive pupal stage. The larvae must come to the surface of the water to breath (with the exception of a few specialized mosquitoes). Mosquito larvae have a siphon at the tail end of the body (Fig. 3). The siphon permits larvae to breathe by penetrating the surface of the water to access air directly.
After the fourth larval instar, the inactive pupa forms. Pupae, often called “tumblers”, do not feed. Mosquito pupae breathe by using their respiratory “trumpets” (Fig. 4) to draw air directly from the atmosphere. Larvae and pupae can be killed by cutting off their access to air with oils or monomolecular films. The pupal stage is normally quite short (1-2 days), after which the adult mosquito emerges.

The last stage is the only one that gets much public attention─the adults that fly, or specifically, the adult females that bite. After a few days, the adult mosquito emerges from the pupal skin and flies away. Only adult female mosquitoes take blood meals, and the blood is used to produce eggs. Male and female mosquitoes also feed on flower nectar. Male mosquitoes look similar to females but can be identified by having feathery antennae (Fig. 5). The long hairs on their antennae help them to locate flying females. Because male mosquitoes travel shorter distances than female mosquitoes, when you find male mosquitoes the source of water that produced them is likely nearby.
Key Species of Mosquitoes in Urban Settings of Arizona
Although there are about 150 species of mosquitoes in the United States and over 40 in Arizona, only a few are problems for urban residents. There are two main types of mosquitoes in Arizona: Stagnant water mosquitoes (Culex mosquitoes) and flood water mosquitoes. In addition, an exotic species of mosquito known as Aedes aegypti, while not native to Arizona, have spread into many populated urban areas of the state. Here we focus on the six key mosquito species important to human and animal health issues in Arizona:
1) Western encephalitis mosquito, Culex tarsalis;
2) Southern house mosquito, Culex quinquefasciatus;
3) Yellow fever mosquito, Aedes aegypti;
4) Malaria mosquito, Anopheles freeborni;
5) Inland floodwater mosquito, Aedes vexans;
6) Dark ricefield mosquito, Psorophora columbiae.
1) Western encephalitis mosquito, Culex tarsalis
Culex tarsalis, or Western encephalitis mosquito (Fig. 6), is the most important vector of arboviruses (refer to a group of viruses that are transmitted by arthropod vectors) in western North America including Arizona. It has a prominent white band across the piercing mouthparts (proboscis) and two white bands across all lower legs. It is the primary vector of West Nile virus, Western equine encephalitis, and St. Louis encephalitis. This mosquito breeds in nearly every freshwater source except tree holes and is commonly found in areas using flood irrigation. Adults can be found in diverse places such as vegetation, ground burrows, barns and culverts. They feed on birds and mammals including humans. In fact the Western encephalitis mosquito, Culex tarsalis will fly 2-10 miles (sometimes much further) in search of a blood meal (Olkowski 1991).
2) Southern house mosquito, Culex quinquefasciatus
Culex quinquefasciatus, more commonly called the Southern house mosquito (Fig. 7), is found throughout the southern half of the United States and can be identified by the five lines that can be seen on the abdomen. It is an annoying pest at night, not only due to its bite but also its distinct high-pitched buzz that announces its presence.
The female Culex quinquefasciatus mosquitoes lay 6-7 broods (egg clusters) each containing ~300 eggs in her six weeks of life (Marin/Sonoma Mosquito & Vector Control District website, Cotati, CA). The southern house mosquito can transmit nematodes that cause dog heartworm and viruses causing encephalitis diseases in humans. As adults they have arrange of 1-5 miles from their origin (Olkowski 1991).
Both species of Culex females deposit their eggs on the water’s surface in tight groupings, or rafts (Fig. 2B). The females’ preferred egg-laying habitats include nearly every source of standing water ranging from small sources, such as mud-puddles, bird baths, outdoor trash cans, landscape ponds, pet water dishes/troughs, and empty flower pots, to larger sources such as school playing fields, over-irrigated lawns, drainage ditches, septic tanks and wells (Gouge 2004a, b). Agricultural fields and other flood-irrigated fields also can support high populations of Culex mosquitoes (Gouge 2004a, b).
As for disease, the West Nile and St. Louis encephalitis viruses are vectored by both Culex species from infected birds, and transmitted to humans (an incidental host) (CDC). Both Culex species feed on birds and mammals, making transmission of the viruses between bird and human hosts more common where the virus is present. Culex tarsalis is especially recognized for vectoring West Nile virus and populations of this mosquito are being monitored by the Arizona Department of Public Health.
3) Yellow fever mosquito, Aedes aegypti
Aedes aegypti, or yellow fever mosquito (Fig. 8), is from the tropics, and responsible for transmitting several diseases in humans and dog heartworm. The diseases in humans include West Nile virus (CDC), yellow fever (not occurring in the US), and dengue fever (occurring in some southern US states but not in Arizona). This mosquito can be identified by the white bands on the hind legs and distinct white lyreshaped markings on the body.
The yellow fever mosquito Aedes aegypti is not native to the desert Southwest and has been spreading into many populated areas of Arizona. It is dependent on human environments for its food and breeding habitat. Unlike our native Culex mosquitoes, A. aegypti lives in close association with human habitations and appears to disperse much less than most other mosquitoes. This is probably based on the availability of egg-laying sites and the ability to obtain human blood (yards not miles). Its flight range is usually 5 -100 meters, although sometimes it may be capable of flying longer distances ─as far as 850 meters or about half a mile (Reiter et al. 1995).
Its native breeding habitat is tree holes, but in Arizona and other introduced areas the female lays eggs on the sides of artificial containers such as old tires, flower pots, barrels, cans, ornamental ponds, and various containers that hold a limited quantity of water (Bennett et al. 2003). Eggs are laid singly (Fig. 2A) on the ground on a moist surface just above the water line, and they hatch when water level is raised by a rain, or an overhead sprinkler, etc. Aedes aegypti eggs are very resilient. They can withstand dry conditions for up to a year, and resume development when water becomes available (Womack 1993). Once they hatch the larvae develop in a relatively short time depending on the temperature. Adult females often bite around the ankles throughout the day, especially early evening. So far their documented range in Arizona extends from the southeast Mexico border to north of Phoenix.
4) Malaria mosquito, Anopheles freeborni
Anopheles freeborni, or the malaria mosquito (Fig. 9), is the most important vector of malaria in Arizona and California. The mosquito also transmits West Nile virus to humans (CDC), avian malaria to bird species and the Myxomatosisvirus to rabbits. This species transmitted malaria in Arizona until the disease was eradicated in the early 1900’s. Since then integrated pest management strategies have enabled us to keep this mosquito under control.
Larvae of this species prefer clear, fresh seepage water in sunlit or partially shaded pools. Roadside ditches and grassy fields provide overwintering sites for adults. The malaria mosquito feeds aggressively on humans, and it bites rabbits, cattle, horses, and dogs as well.
5) Inland floodwater mosquito, Aedes vexans
Aedes vexans, or the inland floodwater mosquito (Fig. 10), is one of the most widespread pest mosquitoes in the world and is found throughout the United States. Inland floodwater mosquitoes are vicious biters and are responsible for most mosquito nuisance complaints. They are recognized as the most serious pest mosquitoes due to their abundance, widespread distribution and breeding potential in floodwater habitats. They are known vectors of West Nile virus (CDC), Western equine encephalitis, St. Louis encephalitis, and dog heartworm. This mosquito is most active at sundown when they attack humans and animals in swarms. The adults are brown with pale V-shaped marks on their abdomens (Fig. 10).
Aedes vexans eggs are laid on soil in areas that have a history of standing water and where they could lay dormant until flooded by water from the next rain or irrigation, allowing the eggs to hatch and larvae to grow and develop in temporary pools. Only one generation is produced per flooding. Their larvae are numerous in these floodwater habitats─irrigation or rainwater that ponds and stands for more than three days ─such as over-irrigated or poorly leveled yards and pastures, tail-water ponds, desert ponds, stock tanks, backed up washes and flood control drainage areas. In most cases, this abundant mosquito will dominate these floodwater habitats. Aedes vexans has a propensity to disperse and can cause nuisance far from its breeding habitat. They may fly more than 10 miles from their larval development sites in search of blood meals.
6) Dark ricefield mosquito, Psorophora columbiae
Psorophora columbiae, or the dark ricefield mosquito (Fig. 11), has a broad range of warm-blooded animal hosts but appears to have a preference for bovine blood. It has been reported to kill livestock when they are in large numbers. The females are furious biters during day or night. Welldocumented studies of cattle have demonstrated severe losses in weight gain and milk production resulting from the blood-feeding activity of this mosquito. The mosquito is an important vector of West Nile Virus in humans (CDC), Venezuelan equine encephalitis and anaplasmosis in cattle.
The adult Psorophora columbiae is a large dark mosquito with white or yellowish markings on its abdomen (Fig. 11). The legs and mouthparts are dark brown and banded with white scales. The hind femora have an apical white band and white knee spots. The first segment of the hind tarsus is brown with a white ring in the middle. The wings are speckled dark brown and white.
Female mosquitoes lay eggs on moist soil that is subject to flooding by water from rainfall or irrigation. The incubation period is about 3-5 days in the rice growing areas of Arkansas. The larvae mature rapidly during the hot summer, often developing from first instar to pupae in as few as 3.5 days. The larvae develop in temporary shallow freshwater pools and puddles where there is vegetation and may occasionally be found in slightly brackish water. Ideal sites for production of larvae are lawns and athletic turf, grassy roadside ditches, and grassy swales (Meisch 1994).
Diseases Spread by Mosquitoes in Urban Areas of Arizona
West Nile Virus (WNV)
West Nile Virus is a mosquito-borne virus contracted through mosquito bites. All six species of mosquitoes mentioned above are potential vectors for West Nile virus. The bites generally happen at dusk and dawn, indoors, in shady areas, or when the weather is cloudy. People of all ages (including children) can contract the virus. About 20% of those who contract WNV will come down with what is called “West Nile fever”; the other 80% of those infected show none or only mild symptoms of the virus. Symptoms of West Nile fever can include: fever, headache, body aches, swollen lymph glands, tiredness and rash on the trunk of the body (Gouge 2012).
About one out of every 150 people with West Nile Virus will develop a severe infection resulting in encephalitis (inflammation of the brain) or meningitis (inflammation of the lining of the brain and spinal cord). Unlike West Nile Fever, which develops with equal likelihood in persons of any age, the severe infection forms tend to occur more in people over 50 years of age. Symptoms of encephalitis or meningitis include: high fever, neck stiffness, disorientation, muscle weakness, paralysis, headache, stupor, tremors, convulsions and coma.
Transmission Cycle of West Nile Virus
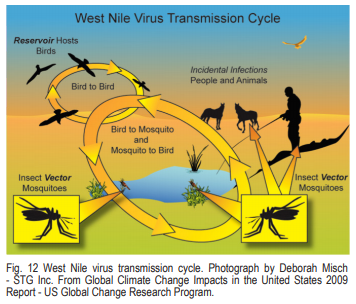
After a mosquito feeds on the blood of a bird infected with West Nile Virus, the virus undergoes a short growth period before it is capable of being retransmitted to humans – as few as four days for some mosquito species in Arizona. The infected mosquito, full of virus and ready to feed again, will look for a bird, human, or other animal for its next blood meal (Fig. 12). This is the basic transmission cycle of the virus as it moves easily from bird (reservoir host) to mosquito (vector) and then, incidentally, on to humans or other animals. Humans and other animals are considered the incidental hosts for West Nile virus. A mosquito cannot become infected by biting a human or pet infected with West Nile Virus. Therefore, humans or other warm-blooded animals cannot further virus transmission and are referred to as “dead end” hosts for the virus.
Encephalitis
Encephalitis is an inflammation of the brain. The causal virus is primarily transmitted by the mosquito Culex tarsalis. The mosquito transmits the virus to birds, horses, mules and occasionally people. Birds serve as the most important host reservoir for the virus in the disease cycle. During the mosquito season public health officials routinely trap and test mosquitoes for viruses, and undertake sentinel chicken flock testing. The chickens are bled once or twice a month and tested for antigens indicating the presence of viruses. Health officials may also survey local and migrating bird populations to determine the incidence of virus and the potential for transmission. However, this is only usually done under special circumstances such as during severe floods.
Western equine encephalitis (WEE) is known to occur in Arizona. Arizona state livestock officials periodically warn horse owners to make sure their horse vaccinations are up to date for the potentially fatal equine sleeping sickness or Western equine encephalitis. The Arizona Department of Health commonly finds mosquitoes carrying the virus that causes WEE.
Mosquitoes carrying WEE are most common during the summer and early fall months. Symptoms of WEE in horses include neurological signs such as depression and lack of coordination. A sick horse may also go down and not be able stand back up. The illness is fatal in 20-50% of horses that are stricken with the disease. Human symptoms include high fever, convulsions, delirium and other characteristic central nervous system dysfunctions. Medical assistance should be obtained quickly if symptoms occur.
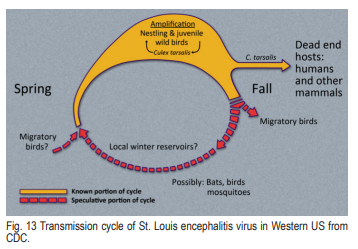
St. Louis encephalitis (SLE) is another viral disease transmitted by Culex tarsalis in Arizona. Birds are again the most important hosts, but humans can also be infected (Fig. 13). Unlike WEE, horses are not involved with the SLE disease cycle. Infected mosquitoes are commonly found in Phoenix, Tucson, Yuma and other sites. Fatal human cases are uncommon and occur sporadically. SLE is a much more serious threat to humans than WEE. Children and the elderly are most susceptible to fatal infections.
Dengue Fever
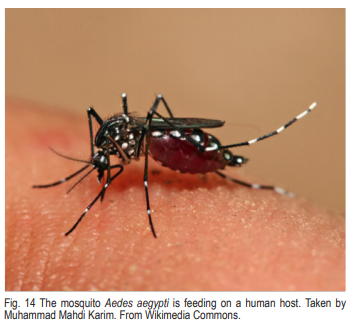
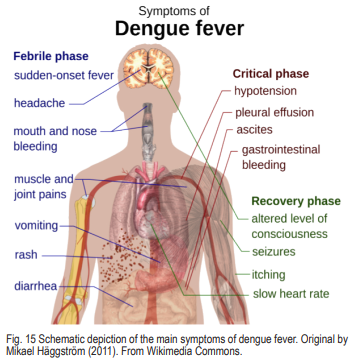
Dengue fever is an infectious disease caused by dengue virus transmitted between humans by Aedes aegypti (Fig. 14). No other animals are involved in the disease cycle. This disease is currently endemic (naturally transmitted) in Mexico and sporadically occurs in southern Gulf States. It is not endemic in Arizona, but this situation is likely to change in the future given the presence of this mosquito throughout Arizona. Dengue fever is characterized by a high fever, a rash, severe muscle and joint pains, and vomiting (Fig. 15). Recovery normally occurs in a few weeks. Dengue hemorrhagic fever and/or dengue shock syndrome are much more serious forms of the disease that occur in people that have had dengue previously. Both hemorrhagic dengue and dengue shock syndrome can be fatal, and children and the elderly are most susceptible.
Dog Heartworm
Mosquitoes also transmit heartworm (Dirofilaria immitis) to dogs. The heartworm is a type of filaria, a small threadlike worm that causes filariasis. Heartworm can cause severe circulatory problems and produce symptoms such as coughing, labored breathing and general loss of vitality in advanced stages.
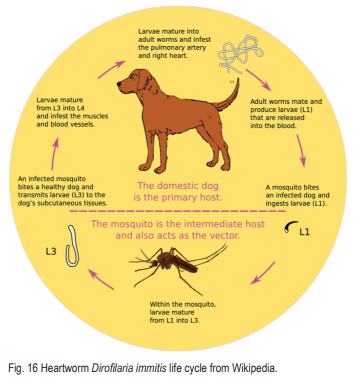
First, adult female heartworms release their young, called microfilariae, into an animal’s bloodstream. Then, mosquitoes become infected with microfilariae while taking blood meal from the infected animal. During the next 10 to 14 days, the microfilariae mature to the infective larval stage within the mosquito. After that, the mosquito bites another dog, cat or other susceptible animal, and the infective larvae enter through the bite wound. Larvae mature into adult worms within about 6 months in heart and blood vessels and then reproduce in the infected dog. In dogs, the worms may live for up to 7 years. Microfilariae cannot mature into adult heartworms without first passing through a mosquito (American Heartworm Society).
Because of the impracticality of protecting dogs from mosquito feeding, the most effective means of controlling heartworm is to prevent worms from reaching the adult stage inside the dog. Veterinarians can prescribe excellent drug treatment to protect pets from heartworm.
Non-chemical Control Measures
1. Prevention Mosquitoes need water to complete their life cycle. They need wet conditions to lay eggs and grow from an aquatic larva into a flying adult. Humans create the vast majority of the wet conditions used by mosquitoes in Arizona. It is likely that many of us have mosquitoes developing in our neighborhood and own backyards. Stagnant water left from monsoon rains and irrigation water can increase mosquito activity and produce hundreds of thousands of mosquitoes if larva are allowed to live as little as three days (Maricopa County Vector Control). Stagnant water in neglected swimming pools is the ideal habitat, though mosquitoes cannot live in a well-maintained swimming pool.
The most effective strategy for mosquito management in communities in general is prevention. The best way to prevent mosquito-borne diseases is to minimize the number of mosquitoes and to prevent them from breeding in the first place. Here are some tips on what you can do to manage mosquitos and eliminate mosquito-breeding sites around you. Consider the following:
1. Check for standing water in plant pots, bird-baths, fountains, tires, tarpaulins covering boats or other objects, and backyard trampolines and other items (Fig. 17A, D). Drain the water regularly (twice a week is ideal). Fig. 17 A. Flush out birdbaths periodically. B. Keep roadside ditches and drainage areas clear of debris so that storm water drains off easily. C. Discard containers that may collect water. D. Avoid prolonged flooding of playing fields. Organic acids can be used to improve turf drainage. A B C D
2. Remove unnecessary clutter. Keep rain gutters free of leaves and other debris that prevent water from draining. Store boats, canoes and other objects so they do not collect rainwater.
3. Repair water leaks (leaky pipes, sprinkler systems, and outside faucets). Correct drainage problems in yards and playing fields. Report drainage problems in ditches (Fig. 17B), etc. Fill holes or depressions in trees with sand.
4. Empty water containers for pets and check livestock watering troughs and tanks (Fig. 17C).
5. Add Gambusia (mosquito eating fish) into personal ponds or stagnant swimming pools to reduce the number of mosquitoes. The fish are available free of charge from the Vector Control office. Just call (602) 506-0700 to schedule a pickup time.
6. Larvicides use bacteria (Bti) that are specifically targeted against the larval life stage of an insect, while harmless to humans, pets and the environment. Mosquito larvicides will kill mosquito larva in a nonconsumptive water source.
2. Avoid Mosquito Bites
Additionally, when outdoors, consider the following safety tips:
1. Wear light colored clothing with loose fitting longsleeves, long pants and socks. Use protective clothing when exposure to mosquitoes cannot be avoided.
2. If possible, avoid outdoor activity before dawn and after dusk when mosquitoes are most active and avoid being bitten by mosquitoes at any time.
3. Properly apply insect repellant even if you are outside for just a short period of time, and share your insect repellant with those around you. For additional help selecting which repellant is right for you, go to the EPA search page: http://cfpub.epa. gov/oppref/insect/#searchform
4. Use a DEET product or a good non-DEET alternative (organic all natural or plant-based insect repellent), and, if you are outside for more than a few hours, reapply repellent frequently. The higher the temperature the more frequently you must reapply repellent for it to be effective.
• Apply repellents only to exposed skin and/or clothing (as directed on the product label). Do not use under clothing.
• Never use repellents over cuts, wounds, or irritated skin.
• Do not apply to eyes and mouth, and apply sparingly around ears. When using sprays do not spray directly onto face; spray on hands first and then apply to face.
• Do not allow children to handle the products, and do not apply to children’s hands. When using on children, apply to your own hands and then put it on the child.
• Do not spray in enclosed areas. Avoid breathing a repellent spray, and do not use it near food.
• After returning indoors, wash treated skin with soap and water or bathe. If you suspect that you or your child is reacting to an insect repellent, discontinue use, wash treated skin. Call your local poison control center if symptoms persist.
• When properly used, personal repellents can discourage biting arthropods from landing on treated skin or clothing.
• Using repellent and sunscreen products at the same time is acceptable practice. However, the use of combination products that contain both an insect repellent and a sunscreen is not recommended.
5. Type of repellents: According to the Centers for Disease Control and Prevention (CDC) the three most common active ingredients in repellents are DEET, picaridin, and oil of lemon eucalyptus. The CDC considers DEET and picaridin to be the most effective. Between the two active ingredients, picaridin products are less problematic when used repeatedly over extended periods of time. EPA characterizes the active ingredients DEET and picaridin as conventional repellents and oil of lemon eucalyptus, PMD, and IR3535 as biorepellents, which are derived from natural materials. For more information on repellent active ingredients, see http://www2.epa.gov/mosquitocontrol.
3. Mosquito-Proof Your Home and Yard
Drain Standing Water: Mosquitoes lay their eggs in standing water. Limit the number of places around your home for mosquitoes to breed by getting rid of items that hold water (Fig. 17A, C, D).
Install or Repair Screens: Some mosquitoes like to come indoors. Keep them outside by having well-fitting screens on both windows and doors. Offer to help neighbors whose screens might be in bad shape. Do not prop doors or keep doors open, particularly early or late in the day when mosquitoes are most active.
Check for Indoor Breeding Sites: If a female mosquito wonders inside your home she will utilize any water reservoir she can find. Check for wriggling larvae in the toilet cisterns that are not flushed daily. Maintain water in drain traps. Use sticky tape over floor drains, sink over flows, etc. to see if you can catch mosquitoes emerging from areas you cannot see.
4. After-Bite Care
Consider the following tips for relieving the itch of mosquito bites:
The first step is to clean the bite area with soap and water. Topical corticosteroids can reduce the rash, itching, and discomfort. Topical diphenhydramine and caine-containing derivatives should be avoided because of concerns about inducing allergic contact sensitivity. Oral antihistamines can be effective for reducing the symptoms of mosquito bites. Use of a cold compress can be helpful, but do not apply ice directly to the skin.
Toxicology and Chemical Control
Effective mosquito control can often be complex and expensive, and frequently requiring the cooperative efforts of communities as well as such groups as industry, agriculture, state and local governments. Many people are concerned about harmful effects of pesticides on the environment, their animals and plants, and themselves. Pesticide toxicity and pesticide hazard is not the same thing. “Toxicity” is the “killing power” under experimental conditions, whereas “hazard” is the risk of poisoning when a product is normally used. Hazard includes both the chemical toxicity and the chance of exposure to the product.
The dosage used and the type of chemical compound determines the hazard level of the pesticide. For example, if an individual were to consume an oral dose of 400 milligrams of table salt per kilogram of body weight the person would become violently ill. In fact every year about 60 people die from aspirin overdose. At lower doses both aspirin and salt are not hazardous. Thus, it is important that the dosage levels recommended on pesticide labels be followed very carefully.
Adulticides
Adulticides are pesticides used to kill adult mosquitoes. Mosquito control districts in the U.S. commonly use adulticides such as permethrin, piperonyl butoxide, and etofenprox. Applications of over-the-counter synthetic pyrethroids applied to vegetation, tree trunks and walls of buildings and catch basins will help control certain adult mosquito species but not others.
Larvicides
Larvicides are products that are used to control mosquitoes in their larval stage and include the following:
1. Bacillus thuringiensis israelensis
Bacillus thuringiensis israelensis, or Bti, is a naturally occurring soil bacterium. The bacterium produces proteins in a crystalline form. When the mosquito larvae eat these crystals, the proteins attack their gut wall, killing the larvae. Bti has a highly specific mode of action, and is of minimal environmental concern. It is quickly biodegraded and leaves no residue. Always store Bti products under cool conditions prior to use.
2. Bacillus sphaericus
Bacillus sphaericus (Bs) is a common soil-inhabiting bacterium. The bacterium produces a protein toxin that may be used to control mosquito larvae. Bs is commonly used to control mosquito larvae in highly polluted water, such as sewage treatment plants. Bs is nontoxic to non-target organisms. Some natural recycling of this organism is likely and products usually last for about 21 days.
3. Spinosad (a mixture of spinosyn A and spinosyn D)
Spinosad insecticide is derived from a family of natural products obtained by fermentation of bacteria species Saccharopolyspora spinosa. This insecticide contains a mixture of two spinosoids, spinosyn A and spinosyn D. Spinosad has high efficacy, a broad insect pest spectrum, low mammalian toxicity, and a good environmental profile. It kills insects via hyperexcitation of the insect nervous system.
4. Methoprene
Methoprene is a synthetic pesticide that mimics the insect juvenile hormone. When methoprene is present, the development of the mosquito larvae is disrupted, and they do not develop to the adult stage. Mosquito control districts use methoprene in situations like cisterns and abandoned swimming pools. The breeding site needs to be treated periodically depending upon the formulation of the product used. Thirty day and 150-day briquettes are available as well as granular formulations (lasting a few days). The compound is not destroyed by heat. Methoprene is toxic to some other insects but is safe for use around humans.
5. Temephos
Temephos is an organophosphate larvicide and used to treat water infested with disease-carrying insects, including mosquitoes, midges, and black fly larvae. Temephos affects the central nervous system through inhibition of cholinesterase. In larvae, this results in death before reaching the adult stage. It is commonly used in areas of standing water where yellow fever mosquito Aedes aegypti breeds in order to reduce the population of this disease-carrying insect.
Alternatives to Pesticides
Oils and monomolecular surface films are used to control pupae and late-fourth instar larvae by interfering with their ability to breath. These products are usually used when an adult emergence will occur without treatment (at this point it is usually too late to utilize the other options). However, oils and monomolecular films will control all immature stages.
Gambusia is mosquito-eating fish. Some mosquito control districts raise the fish and use them to stock man-made water bodies. These fish will reproduce and continue to eat mosquito larvae. Gambusia should never be released into natural watercourses as they out compete native fish species. The Gila topminnow is now a protected fish because of competition with Gambusia. In many areas where Gambusia have been released the Gila topminnow no longer exists. Most small minnow fish (such as guppies, flathead minnow and shad) are good at reducing mosquito larvae populations and are suitable for release into garden ponds.
Area-wide Mosquito Control
Because of the complexity of controlling mosquito populations, technical assistance may be required. Mosquito control personnel may be necessary on a permanent basis and communities may wish to investigate the desirability of an area-wide approach.
The most important element in mosquito control is you. By reducing mosquito-breeding habitats on your property you can significantly reduce mosquito populations with no side effects.
In Summary: Some Final Facts
• There are 150 different species of mosquitoes occurring in the United States and over 40 species in Arizona.
• A single female can lay hundreds of eggs over her lifetime.
• Aedes aegypti eggs can survive for more than five years under certain conditions.
• All mosquitoes need water to complete their life cycle.
• Not all species bite humans; some prefer birds, others prefer horses.
• Only females take a blood meal; both males and females feed on plant nectar.
• Some mosquito species fly considerable distances, 20 miles or more. Some species tend to remain close to their larval habitats.
• Adult females can survive several weeks.
• Mosquitoes are responsible for more human mortality around the world than any other living creature