
School & Home Integrated
Pest Management (IPM)
Newsletter – May 2017
View this newsletter as a PDF.
Editor: Shujuan (Lucy) Li, lisj@cals.arizona.edu
Dawn H. Gouge1,2, James Hagler3, Shaku Nair2, Kathleen Walker1, Shujuan (Lucy) Li2, Christopher S. Bibbs4, Chris Sumner5 Kirk A. Smith6
1Department of Entomology - College of Agriculture & Life Sciences, University of Arizona; 2Cooperative Extension - Arizona Pest Management Center, University of Arizona; 3Arid Land Agricultural Research Center, USDA; 4Anastasia Mosquito Control District, FL; 5Yuma County Pest Abatement District, AZ; 6Maricopa County Environmental Services Department, Vector Control Division, AZ
There are a number of disease-causing viruses transmitted to people primarily through the bite of infected mosquitoes. Female mosquitoes take blood meals to produce eggs (Fig. 1). A mosquito that bites an infected animal may pick up a virus within the blood meal. If the mosquito is the appropriate species, and conditions inside the insect and the surrounding environment are supportive, the virus reproduces within the mosquito. Later, the mosquito may pass the virus on to other animals (including humans) as they feed again.
 Not all mosquitoes vector (transmit) viral diseases to humans, and specific mosquito species vector specific viruses. The successful replication and transmission of viruses in mosquitoes depends on several factors, the most important being the compatibility of the vector, ambient temperature and humidity (higher temperatures often accelerate virus replication), and mosquito life span. Some arboviruses (arthropod-borne, primarily insects and ticks) such as St. Louis encephalitis virus and western equine encephalitis virus have been present in the United States for many years. Others are relatively recent introductions, such as West Nile virus, and many more are emerging as public health threats, including dengue virus, chikungunya virus, and Zika virus. The increasing circulation of arboviruses that threaten human health (Fig. 2) may be due to many factors including: climate change; wildland-urban interface population increases; globalization trends; widespread use of plastic containers and packaging (which provides habitat for species that breed in manmade water-holding containers); decreased funding for research and vector control; the development of pesticide resistance; and a lack of new management tools.
Not all mosquitoes vector (transmit) viral diseases to humans, and specific mosquito species vector specific viruses. The successful replication and transmission of viruses in mosquitoes depends on several factors, the most important being the compatibility of the vector, ambient temperature and humidity (higher temperatures often accelerate virus replication), and mosquito life span. Some arboviruses (arthropod-borne, primarily insects and ticks) such as St. Louis encephalitis virus and western equine encephalitis virus have been present in the United States for many years. Others are relatively recent introductions, such as West Nile virus, and many more are emerging as public health threats, including dengue virus, chikungunya virus, and Zika virus. The increasing circulation of arboviruses that threaten human health (Fig. 2) may be due to many factors including: climate change; wildland-urban interface population increases; globalization trends; widespread use of plastic containers and packaging (which provides habitat for species that breed in manmade water-holding containers); decreased funding for research and vector control; the development of pesticide resistance; and a lack of new management tools.

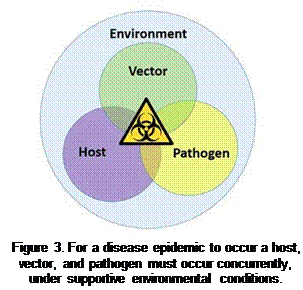
In order for a disease epidemic to occur, a susceptible host, a competent vector, and a pathogen must be together in the same place, at the same time, and under supportive environmental conditions (Fig. 3). While children and the elderly are most severely impacted by mosquito-borne pathogens, in some instances life-threatening illness or permanent debilitation can occur in hosts of any age.
West Nile virus is vectored by Culex tarsalis and Culex quinquefasciatus, the latter being the predominant vector in Arizona. Mosquitoes become infected when they feed on infected birds, and can transmit the virus to other birds during later blood meals, the virus may be injected into humans and other animals, where it can cause illness. Of all the arbovirus disease cases, West Nile Fever has the highest case counts in Arizona to date. Infected mosquitoes are found throughout the state.
The virus can affect people of all ages, with 2030% of those infected developing West Nile fever, and the rest showing mild or no symptoms. The incubation period (the time from infected mosquito bite to onset of illness) is 3 to 14 days if symptoms develop at all. The virus may also be transmitted through contact with bodily fluids from other infected animals. Human infections have also occurred through organ transplant, blood transfusions and breast milk. There are very few reports of transplacental (mother to developing fetus) transmission. To date, no human-to-human transmission through normal contact has been reported.
West Nile fever symptoms include: fever, headache, body aches, swollen lymph glands, tiredness and rash on the trunk of the body. About one out of every 150 people infected with the West Nile virus will develop a severe infection resulting in encephalitis (inflammation of the brain), or meningitis (inflammation of the lining of the brain and spinal cord). Unlike West Nile fever, which develops with equal likelihood in persons of any age, the severe neuroinvasive form tends to occur more in people over 50 years of age.
Symptoms of encephalitis or meningitis include high fever, neck stiffness, disorientation, muscle weakness, paralysis, headache, stupor, tremors, convulsions and coma. Death can result.
While there is no vaccination against West Nile virus for humans, there are a number of vaccinations for equine use. Some protect specifically against West Nile virus, while some vaccinate against a number of equine pathogens. Veterinarians highly recommend horses receive West Nile vaccinations as the virus causes fatal disease in a third of infected horses, and annual boosters are required to maintain immunity.
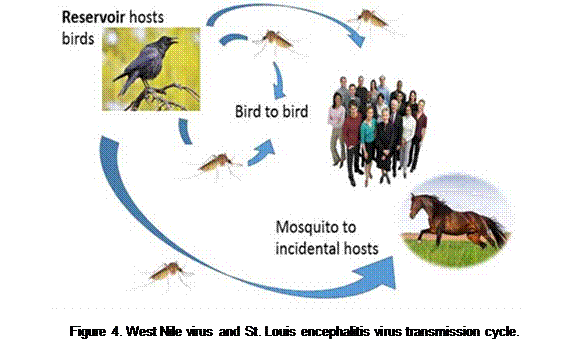
St. Louis encephalitis virus is another disease-causing virus vectored by Culex tarsalis and Culex quinquefasciatus mosquitoes in Arizona. Birds again are the primary hosts, but humans can also be infected (Fig. 4). Infected mosquitoes are commonly found in Phoenix, Tucson, Yuma and other cities.
The incubation period for St. Louis encephalitis disease ranges from 5 to 15 days. Fatal human cases are uncommon but a significant number of human clinical cases were recorded in Arizona during 2015. Less than 1% of St. Louis encephalitis virus infections are clinically apparent most infections going undiagnosed. However, St. Louis encephalitis virus generates a higher incidence of neuroinvasive cases compared with West Nile virus, and children and the elderly are the most severely impacted. About 40% of children and young adults with St. Louis encephalitis disease develop a fever, headache or aseptic meningitis, and about 90% of elderly with St. Louis encephalitis disease develop encephalitis. The risk of fatal disease increases with age. Unfortunately, there is no vaccination available for St. Louis encephalitis virus.
Exotic viruses that if introduced could be vectored by Arizona mosquito species
None of the exotic viruses listed here are endemic (naturally transmitted) within Arizona at the time of this writing, but given that we have one of the vector mosquitoes, and travelers contracting the virus and returning to Arizona regularly, this situation may change at any time. In all cases, humans are the primary host and Aedes aegypti and Aedes albopictus (not currently established in Arizona) are potential vectors.
Chikungunya virus is transmitted rarely from mother to newborn around the time of birth but this virus is not spread from person to person.
 Outbreaks of chikungunya have been reported from countries in Africa, Asia, Europe, Indian and Pacific Ocean islands. The virus arrived in the Americas in late 2013 on the island of St. Martin and local transmission spread it quickly through the Caribbean and into South and Central America. Local transmission (Fig. 5) means that mosquitoes in the area have been infected with the virus and are spreading it within the local population. Beginning in 2014, chikungunya disease cases were reported among United States travelers returning from affected areas in the Americas and local transmission was identified in Florida, Puerto Rico, and the Virgin Islands. During 2016, travel-related chikungunya cases were reported in 37 of the continental states, including
Outbreaks of chikungunya have been reported from countries in Africa, Asia, Europe, Indian and Pacific Ocean islands. The virus arrived in the Americas in late 2013 on the island of St. Martin and local transmission spread it quickly through the Caribbean and into South and Central America. Local transmission (Fig. 5) means that mosquitoes in the area have been infected with the virus and are spreading it within the local population. Beginning in 2014, chikungunya disease cases were reported among United States travelers returning from affected areas in the Americas and local transmission was identified in Florida, Puerto Rico, and the Virgin Islands. During 2016, travel-related chikungunya cases were reported in 37 of the continental states, including
Arizona, but no local transmission has occurred in Arizona to date.
The majority of people infected with chikungunya virus will develop some symptoms which develop 3–7 days after being bitten by an infected mosquito. People infected with chikungunya virus typically develop fever and joint pain, which can be extremely severe as the virus cases arthritogenic disease (causing joint pain). Other symptoms can include muscle aches, headaches, nausea, vomiting, joint swelling and rash. Travelers returning from areas with local transmission of chikungunya virus should seek medical care if they experience any of these symptoms. Healthcare providers in areas with reported cases should be on the alert for local transmission.
Infection with chikungunya virus is rarely fatal, but the joint pain can often be severe and debilitating. Patients recover in about a week, although long-term joint pain occurs in some people. According to the CDC, infection is thought to provide lifelong immunity.
During 2016, researchers developed the first chikungunya vaccine that may be approved for use at some point in the future.
Dengue virus causes dengue fever (Fig. 6), an infectious disease caused by any one of five related dengue virus serotypes (variations). Dengue virus is currently endemic (regularly transmitted) in more than 100 countries including many popular tourist destinations in Mexico, Puerto Rico, Latin America, Southeast Asia, Africa and the Pacific Islands. Cases occur regularly in southern Gulf States of the United States (Texas, Louisiana, Mississippi, Alabama, and Florida).
More than one-third of the world population live in areas with the virus and its vector, and dengue is a leading cause of illness and death in the tropics and subtropics, with estimates of 400 million people infected annually. Dengue can be transmitted in organ transplants and blood transfusions from infected donors, and between an infected pregnant mother and her fetus.

Figure 6. The course of infection and symptoms resulting from various stages of dengue.
The incubation period is 4–7 days and the majority of people infected develop symptoms lasting between 3–10 days. It has been established that even asymptomatic infections (infected people with no symptoms of illness) generate a high enough level of viremia (virus particles) in their blood to provide feeding mosquitoes with virus, which can sustain high levels of transmission.
Symptoms of dengue fever include high fever, rash, severe headache, severe muscle and joint pains, mild bleeding from the skin, nose, and gums, and vomiting. Most people recover from dengue infections within a few weeks. Dengue fever results from infection by one of the dengue serotypes, but infection by one serotype does not generate an immunity to the others, and ongoing infections put people at greater risk for the far more serious forms of the disease dengue hemorrhagic fever, and dengue shock syndrome. Both severe forms of the disease can be fatal, and children and the elderly are the most at risk.
Dengue fever mortality rate is typically less than 1% of symptomatic cases. When treated, dengue hemorrhagic fever has a mortality rate of 2-5%, but if left untreated, the mortality rate may be 50%. There are no vaccines to prevent dengue virus infection available in the United States currently, but the DENGVAXIA® vaccine has been approved in Mexico and many other countries.
Zika virus infections in humans have been documented since 1952, but the first large outbreak of Zika was reported on the Island of Yap in 2007. Zika was identified as a global health concern in 2015 when an outbreak in Brazil was linked to a dramatic increase in cases of babies born with microcephaly (Fig. 7).
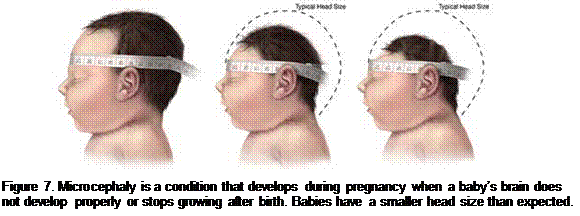
Microcephaly is a neurological condition in which the brain develops abnormally in the womb, and an infant’s head is smaller than the heads of other babies of the same sex and age. Currently, locally acquired Zika disease cases have been reported in many countries, several United States territories, Texas, and Florida. For up to date information on Zika cases reported around the world go to https://www.cdc.gov/zika/geo/.
As well as transmission via the bite of a mosquito, Zika virus can also be transmitted from mother to fetus during pregnancy, through blood transfusions, bodily fluids, and by sexual contact. At this point three Aedes species have been found capable of vectoring the Zika virus (Aedes vexans, in addition to Aedes aegypti, and Aedes albopictus).
The incubation period is typically 2-7 days, and about 20% of people infected with Zika virus become ill and develop Zika symptoms. The most common symptoms are fever, rash, joint pain, and/or conjunctivitis (red eyes) (Fig. 8). Other symptoms include muscle pain and headache. The illness is usually mild, with symptoms lasting for a few days to a week. Severe disease symptoms requiring hospitalization are uncommon. Death due to the virus is rare. The main health concerns are related to pregnant women and impacts on the developing fetus.

Congenital Zika syndrome is a pattern of birth defects occurring when babies are infected with Zika virus during pregnancy. Birth defects include: severe microcephaly where the skull is partially collapsed, decreased brain tissue, damage to the back of the eye, joints with limited range of motion, muscle abnormalities restricting body movement. Some infants with congenital Zika virus infection who do not have microcephaly at birth may later develop postnatal microcephaly. Recognizing that Zika is a cause of certain birth defects does not mean that every pregnant woman infected with Zika will have a baby with a birth defect.
However, infection with Zika during pregnancy increases the chances of birth defects, and infection during the first trimester is particularly problematic. The CDC does not believe that a woman who has fully recovered from a past Zika virus infection (and who no longer has Zika virus in her blood) is at greater risk for birth defects in future pregnancies. However, there is still much we need to learn about this virus and the pathology of Zika infection. Check https://www.cdc.gov/zika/pregnancy/index.html for the latest information.
See a healthcare provider if you develop symptoms, particularly if you have visited an area where Zika is common: http://wwwnc.cdc.gov/travel/page/zika-travel-information. If you have recently traveled, tell your healthcare provider where and when you traveled. Your blood may be tested for Zika virus and other viruses that cause similar symptoms like dengue and chikungunya viruses. Work on a Zika vaccine is underway, but it could be several years before one is available.
The most effective way to avoid arbovirus illness is to avoid mosquito bites.
It is particularly important for women of childbearing age to avoid mosquito bites – cover up, use insect repellents, and keep indoor living space free of mosquitoes.
People infected with any of the arboviruses should protect themselves from additional mosquito bites by wearing insect repellents, using air conditioning, or window and door screens to keep mosquitoes out of homes and buildings. Wearing long pants and long-sleeved shirts when possible is also advisable. Protecting yourself and others from mosquito bites during the first few days of illness can help prevent other mosquitoes from becoming infected and reduce the risk of further spread.
For more information about managing mosquito vectors around your home go to: https://extension.arizona.edu/sites/extension.arizona.edu/files/pubs/az1706-2016.pdf
For more information about mosquito biology, ecology and management go to https://extension.arizona.edu/sites/extension.arizona.edu/files/pubs/az1706-2016.pdf